Today, our senior teaching resident reviewed an article from the Journal of Pediatrics titled Comparative Effectiveness of Dexamethasone versus Prednisone in Children Hospitalized with Asthma. This line of research has some interesting implications for primary care and how we manage outpatient asthma exacerbations.
One thing that came up was how dex could be a benefit based only on the fact it doesn’t require the family to pick up a prescription. Can you guess how often families pick up their prescribed meds?
I found a distressing answer in this paper from 2005 in the American Journal of Emergency Medicine that looked at ED discharge prescriptions.

The authors looked at insurance claim data as a marker of prescription pickup compared against ED visit records. These were “high-urgency” prescriptions that would have been expected to be started immediately after discharge. Table 1 says it all:
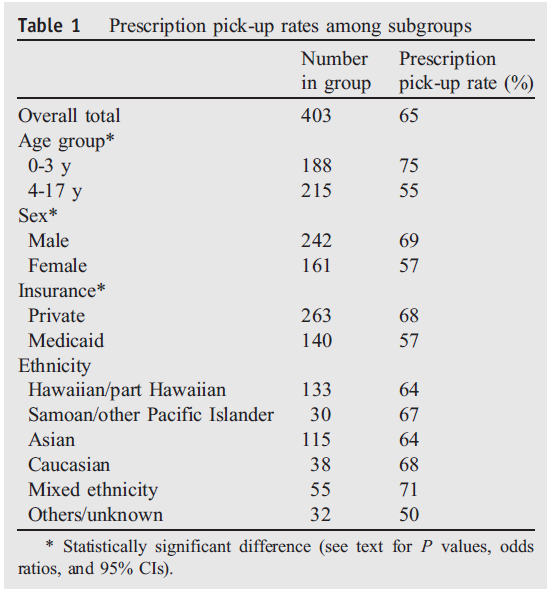
At best, 75% of prescriptions were picked up… oof. You can imagine an intervention like dex, which doesn’t require a pharmacy visit (so long as they already have albuterol), could be an improvement based solely on ease of compliance.
OK, if you can’t hand someone a full course of medication at the time of the visit (few places can do this) and your visit lengths don’t allow you to stop and drive the family to the pharmacy and wait with them for the Rx, what can you do?
Dr. Glick and colleagues have some recommendations based on their 2017 review in Pediatrics: Parental Management of Discharge Instructions: A Systematic Review .
- Pay special attention to return precautions, help families understand signs and symptoms to look for. This is challenging to do well, a great thing to pick the brains of your mentors on.
- Review medication side effects (be sure to know common ones)
- Simple instructions are better, use diagrams, ensure literacy in the language you use!
- Demonstrate measurement of medications – I like to mark syringes and it is helpful to have an idea of how many mLs fit in a measuring cup, OTC Tylenol syringe, etc. E.g. 3.75 mL is an easy measurement with most commercial OTC antipyretics, but harder with a hospital grade 5 mL syringe.
- Have parents teach back instructions – a great strategy to get immediate feedback on how effective your instructions were!
References
Kajioka, E. H., Itoman, E. M., Li, M. L., Taira, D. A., Li, G. G., & Yamamoto, L. G. (2005). Pediatric prescription pick-up rates after ED visits. American Journal of Emergency Medicine, 23(4), 454–458. https://doi.org/10.1016/j.ajem.2004.10.015
Glick, A. F., Farkas, J. S., Nicholson, J., Dreyer, B. P., Fears, M., Bandera, C., … Yin, H. S. (2017). Parental Management of Discharge Instructions: A Systematic Review. Pediatrics, 140(2), e20164165. https://doi.org/10.1542/peds.2016-4165
Parikh, K., Hall, M., Mittal, V., Montalbano, A., Gold, J., Mahant, S., … Shah, S. S. (2015). Comparative Effectiveness of Dexamethasone versus Prednisone in Children Hospitalized with Asthma. Journal of Pediatrics, 167(3), 639-644.e1. https://doi.org/10.1016/j.jpeds.2015.06.038
